As initially described by Borbély and colleagues, the timing of sleep is dictated by two main processes: our circadian rhythm and our homeostatic pressure for sleep.
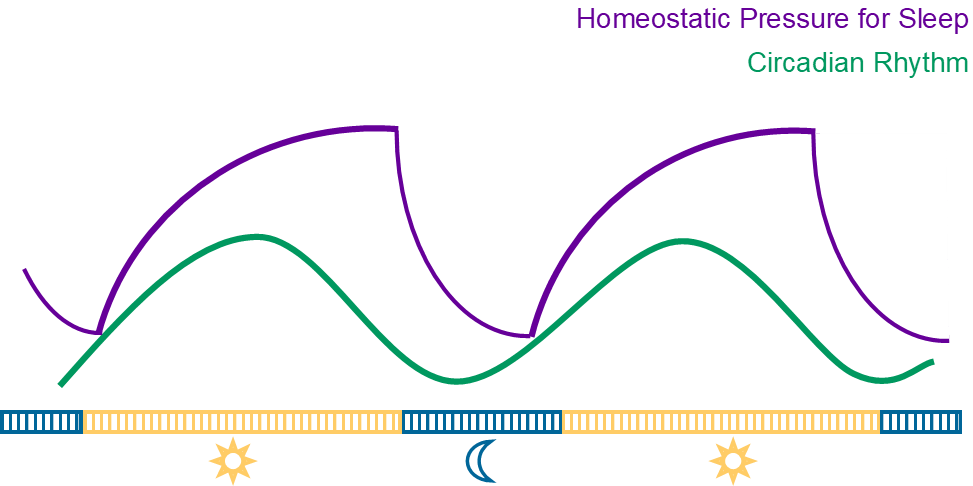
The circadian rhythm (circa = about, diem = day), shown by the green line in the above graph, relates to our internal body clock which controls the rhythmic behavior of our body. This rhythm activity is found in our cell activity, gene expression, hormone secretion, etc.
As humans are diurnal creatures, we are biologically programmed to be awake during the day period and asleep during the night. Light, temperature, eating patterns and other environmental and behavioral cues help keep our internal clock synchronized to the 24-hr day/night cycle. If our bodies become desynchronized, sleep quality becomes disrupted. REM sleep, which is typically found in the later part of the night’s sleep, is particularly linked to our circadian rhythm.
The best example of a desynchronized body clock is what we experience during jet-lag, where our internal clock is still linked to the old time zone, but we physically find ourselves in a new time zone with a different phase of the environmental day/night cycle. Our bodies will eventually adapt to the different time zone, however, this is not an automatic process.
On the other hand, the homeostatic pressure for sleep is a separate phenomenon. Acting like a gauge, and shown by the purple line in the above illustration, it is the accumulated pressure or need for sleep that results from wakefulness. The longer we are awake, the stronger this pressure builds up, and the more we crave sleep, typically at the end of the day. Therefore, the homeostatic pressure is dependent on the preceding wake and sleep period.
Additionally, the deep slow wave sleep of NREM stage 3 is linked to the homeostatic pressure. This means that the greater the pressure for sleep, the more slow wave sleep will be present in the following night’s sleep.
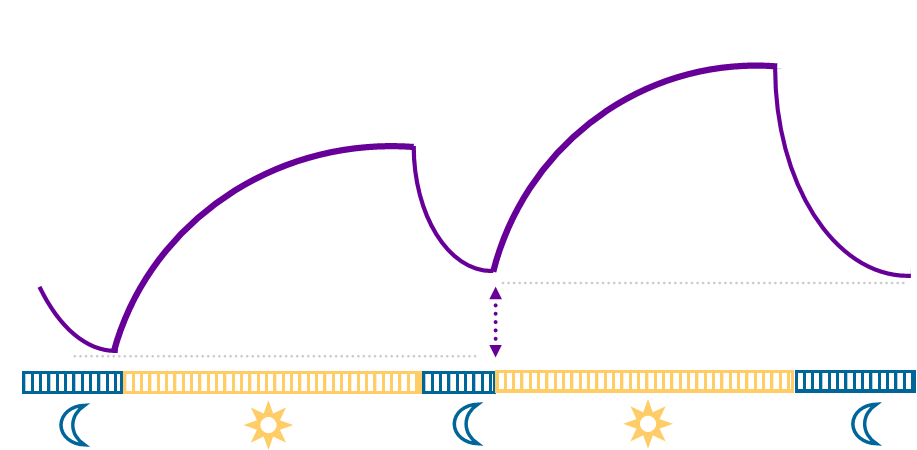
Based on the homeostatic pressure, a night of short sleep will not successfully reset the pressure gauge. Therefore, as shown in the above illustration, the next day, you are not starting the day at ‘0’ and, as a result, will be feeling additionally tired throughout the day.
Likewise, if you nap during the day, this will lessen the accumulated pressure. Although this can bring benefit, it can also result in reduced pressure for sleep come night-time, when your internal clock is telling you it is time to sleep.
Although these are the two main processes dictating the timing of sleep, there are a number of factors that act on the circadian rhythm, the homeostatic pressure, or both. Such factors include your age, activity levels, caffeine intake, stress levels, light exposure, recent travels, health and immune system, and many more. These will be further examined in upcoming sections. Nevertheless, it is important to highlight that there are a number of factors that can modulate the timing of sleep.
Supporting References:
- Borbély, A. A. (1982). A Two Process Model of Sleep Regulation. Human Neurobiology, 1(3), 195-204.
- Achermann, P. (2004). The Two-Process Model of Sleep Regulation Revisited. Aviation, Space, and Environmental Medicine, 75(3), A37-A43.
- Borbély, A. A., & Achermann, P. (1999). Sleep Homeostasis and Models of Sleep Regulation. Journal of Biological Rhythms, 14(6), 559-570.
- Borbély, A. A., Daan, S., Wirz‐Justice, A., & Deboer, T. (2016). The Two‐Process Model of Sleep Regulation: A Reappraisal. Journal of Sleep Research, 25, 131-143.
- Gachon, F., Nagoshi, E., Brown, S. A., Ripperger, J., & Schibler, U. (2004) The Mammalian Circadian Timing System: From gene expression to physiology. Chromosoma, 113(3) 103-112.
- Stephan, F. K., & Zucker, I. (1972). Circadian Rhythms in Drinking Behavior and Locomotor Activity of Rats are Eliminated by Hypothalamic Lesions. Proceedings of the National Academy of Sciences, 69(6), 1583-1586.
- Aubin, S. (2018). L’influence de la cécité sur le rythme circadien et le sommeil.
2 thoughts
Comments are closed.